Infectious Keratitis (corneal ulcer)
Microbial keratitis continues to be a leading cause of ocular morbidity and blindness worldwide, more so in developing countries. Its annual incidence is reported to be 11.3 per 10,000 people in India.
Some common factors contributing to the increased prevalence are ocular trauma, contact lens wear, coexisting ocular diseases, diabetes mellitus, leprosy and injudicious use of topical steroids.
Dry eye
A ‘dry eye’ is a condition where patients suffer from irritation and discomfort in the eye because of the decreased quantity of tears or increased evaporation of tears from the eye. The symptoms are non-specific and can range from a tired or itching eye to diminished vision in severe cases. A clinical examination can help diagnose a condition of ‘dry eyes’ but, to be more definitive, diagnostic tests are required.
The treatment includes use of preservative-free artificial tears, and topical immunosuppressive treatment.
Dry eyes can also be a manifestation of systemic diseases like rheumatoid arthritis and even due to Steven Johnson Syndrome. A blood examination could help identify the disease, which can then be jointly treated by the ophthalmologist and rheumatologist. Patients who have such symptoms are advised procedures to preserve tears through implantation of silicone punctual plugs or cauterizing the puncta (tear glands).
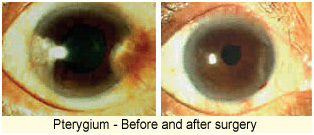
Pterygium
A pterygium is a pinkish, triangular-shaped tissue growth on the cornea. Some pterygia grow slowly throughout a person’s life, while others stop growing after a certain point. A pterygium rarely grows so large that it begins to cover the pupil of the eye.
Pterygia are more common in sunny climates and in the 20-40 age group. Scientists do not know what causes pterygia to develop. However, since people who have pterygia usually have spent a significant time outdoors, many doctors believe ultraviolet (UV) light from the sun may be a factor. In areas where sunlight is strong, wearing protective eyeglasses, sunglasses, and/or hats with brims are suggested. Because a pterygium is visible, many people want to have it removed for cosmetic reasons. It is usually not too noticeable unless it becomes red and swollen from dust or air pollutants.
Pterygium excision is not recommended unless it affects vision. If a pterygium is surgically removed, it may grow back, particularly if the patient is less than 40 years of age. Lubricants can reduce the redness and provide relief from the chronic irritation.
Keratoconus
Keratoconus arises when the middle of the cornea thins and gradually bulges outward, forming a rounded cone shape. It is a progressive disorder affecting one in every 2,000 Indians and is more prevalent in teenagers and adults in their 20s. This abnormal curvature changes the cornea’s refractive power, producing moderate to severe distortion (from astigmatism) and blurriness (from nearsightedness) of vision. Keratoconus may also cause swelling and a sight-impairing scarring of the tissue.
Keratoconus usually affects both eyes. At first, people can correct their vision with eyeglasses. But as the astigmatism worsens, they must rely on specially fitted contact lenses to reduce the distortion and provide better vision. It can also cause increased light sensitivity and glare. Although finding a comfortable contact lens can be an extremely frustrating and difficult process, it is crucial because a poorly fitting lens could further damage the cornea and make wearing a contact lens intolerable. ROSE K are specialized lenses are meant for patients who are unable to adjust to RGP contact lenses.
A new non-surgical, noninvasive treatment, based on collagen cross linking with Ultraviolet A (UVA, 365nm) and riboflavin (Vitamin B 2), a photosensitizing agent is now available for treating keratoconus. This changes the intrinsic biomechanical properties of the cornea, increasing its strength by almost 300%. This increase in corneal strength has shown to arrest the progression of keratoconus in numerous studies all over the world.
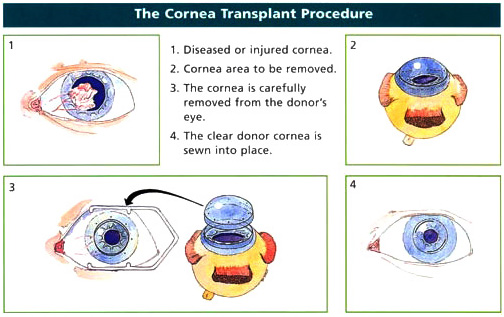
What is Corneal Transplantation?
Corneal transplantation is a procedure in which diseased cornea is surgically removed and replaced with a healthy one to restore clear vision.
The cornea is the front, outermost layer of the eye. Just as a window lets light into a room, the cornea lets light into the eye. It also focuses the light passing through it to make images clear and sharp.
Corneal problems can occur in anyone regardless of age. Sometimes due to disease, injury or infection the cornea becomes cloudy or warped. A damaged cornea, like a frosted or misshapen windowpane, distorts light as it enters the eye. This not only causes distortion in vision, it may also cause pain.
Stem cell and buccal mucosal transplantation
Stem Cell Transplant for Ocular Surface Diseases
The ocular surface comprises the corneal epithelium and the conjunctival epithelium covering the cornea and front surface of the eye. Ocular Surface Diseases (OSD) are the result of injuries to or cell deficiency of the corneal epithelium and conjunctival epithelium, causing blindness. Direct causes include chemical and thermal burns, trachoma and Stevens Johnson syndrome.
Previously, treating OSD with conventional corneal transplants was not very successful because the Limbal Stem Cells (source of healthy corneal epithelium) and Conjunctival Stem Cells were not being transplanted at the same time. Now with newer technologies stem cell transplantation has become more available.
Patients with severe ocular surface damage are advised to undergo limbal stem cell transplantation for the restoration of the ocular surface and the improvement of visual acuity.
Amniotic membrane transplantation
Amniotic membrane transplantation is currently being used for a continuously widening spectrum of ophthalmic indications. It has gained widespread attention as an effective method of reconstruction of the ocular surface. Amniotic membrane obtained from human placenta in a sterile technique has a unique combination of properties, including the facilitation of migration of epithelial cells, the reinforcement of basal cellular adhesion and the encouragement of epithelial differentiation. Its ability to modulate stromal scarring and its anti-inflammatory activity has led to its use in the treatment of ocular surface pathology as well as an adjunct to limbal stem cell grafts. Amniotic membrane transplantation has been used for reconstruction of the corneal surface in the setting of persistent epithelial defects, partial limbal stem cell deficiency, bullous keratopathy and corneoscleral ulcers. It has also been used in conjunction with limbal stem cell transplantation for total limbal stem cell deficiency. Amniotic membrane grafts have been effectively used as a conjunctival substitute for reconstruction of conjunctival defects following removal of pterygia, conjunctival lesions and symblephara. More recently, amniotic membrane has been used as a substrate for ex vivo cultivation of limbal, corneal and conjunctival epithelial cells
Keratoprosthesis
The Keratoprothesis is an artificial cornea that can be used after standard corneal transplant has failed or when such a transplant would be unlikely to succeed. Thus keratoprosthesis implantation is a procedure designed to help blind patients whose conditions are the most difficult to treat.
Development
The Boston Keratoprosthesis has been under development since the 1960s and has been gradually improved. It received FDA clearance in 1992. More than 3,000 implantations have been performed (January 2009). It is the most commonly used artificial cornea in the United States and in the world.
The keratoprosthesis is made of clear plastic with excellent tissue tolerance and optical properties. It consists of three parts and when fully assembled, has the shape of a collar-button.
The device is inserted into a corneal graft, which is then sutured into the patient’s cornea as in standard transplantation. If the natural lens is in place, it is also removed. Finally, a soft contact lens is applied to the surface; it must be worn around the clock, everyday. This does not cause any discomfort.
Our one-step surgery is simpler and faster than procedures used in other keratoprosthesis models; it generally requires about one and one half hours to complete. While general anesthesia is recommended, the recent trend is for performing the surgery under local anesthesia with intravenous sedation. Visual improvement is usually seen the following day or week(s). Although the prosthesis is clear, use of a colored contact lens can perfectly match the iris color of the opposite eye.
Stability and Safety
The Boston Keratoprosthesis is known for excellent long-term (many years) stability and safety. Its optical system can provide normal vision if the rest of the eye is undamaged.
The surgery is reversible at any time.
